
01 Sep Cholesterol: The Good, the Bad, and the Truth!
By: Dr. Robert Irons, Ph.D.
September is Cholesterol Awareness Month. For many years, the only information about high cholesterol has been negative, but, now there are studies supporting some benefits of “high cholesterol”. Before we introduce you to the new information, we’ll provide some background on cholesterol and its essential roles in normal physiology, and discuss how your diet can improve an unhealthy cholesterol status.
What is cholesterol?
Cholesterol is a soft, waxy substance found among fats circulating in your bloodstream and in all of your body’s cells. Cholesterol is a precursor for hormones, requiring only minor modifications to become testosterone, estrogen or vitamin D. Your body needs cholesterol, and it has its own machinery to make it. You can also get cholesterol from animal products you eat, such as: meat, poultry, fish, eggs, butter, cheese, milk, etc. Cholesterol is made only by animals, and is NOT found in foods from plants. It is used as a marker for heart disease or cardiovascular disease. Three components of cholesterol are used for this biomarker: High-Density Lipoprotein (HDL), Low-Density Lipoprotein (LDL) and Triglycerides (TG).
What is “good” cholesterol?
The medical term for “good” cholesterol is high-density lipoprotein (HDL). HDL carries cholesterol away from your arteries and takes it to your liver, where it’s removed from your body. High levels of HDL protect you from heart attacks. Blood HDL levels less than 40 mg/dL for men and less than 50 mg/dL for women may increase your risk for heart disease. HDL levels higher than 60 mg/dL may help protect you against heart disease.
What is “bad” cholesterol?
The medical term for “bad” cholesterol is low-density lipoprotein (LDL). High levels of “bad” cholesterol in your body can clog your arteries and increase your risk of heart attack and stroke. That’s the ugly truth. When there is too much bad cholesterol in your body, it can slowly build up in the walls of the arteries in your heart and brain. Once there, it can combine with other substances to form plaque, which can narrow your arteries, make them less flexible, and restrict blood flow. This is a medical condition called atherosclerosis. If a blood clot forms and blocks an artery narrowed by plaque, it is possible that you could have a heart attack or stroke. For good health, it is recommended to keep your blood LDL low – below 100 mg/dL.
What are triglycerides?
Triglycerides are a form of fat that’s made in your body. People who have high levels of triglycerides often have a low level of “good” cholesterol (HDL) and a high level of “bad” cholesterol (LDL). Blood triglyceride levels of 150 mg/dL or higher may increase your risk for heart disease. Many people with heart disease, diabetes or both have high triglyceride levels.
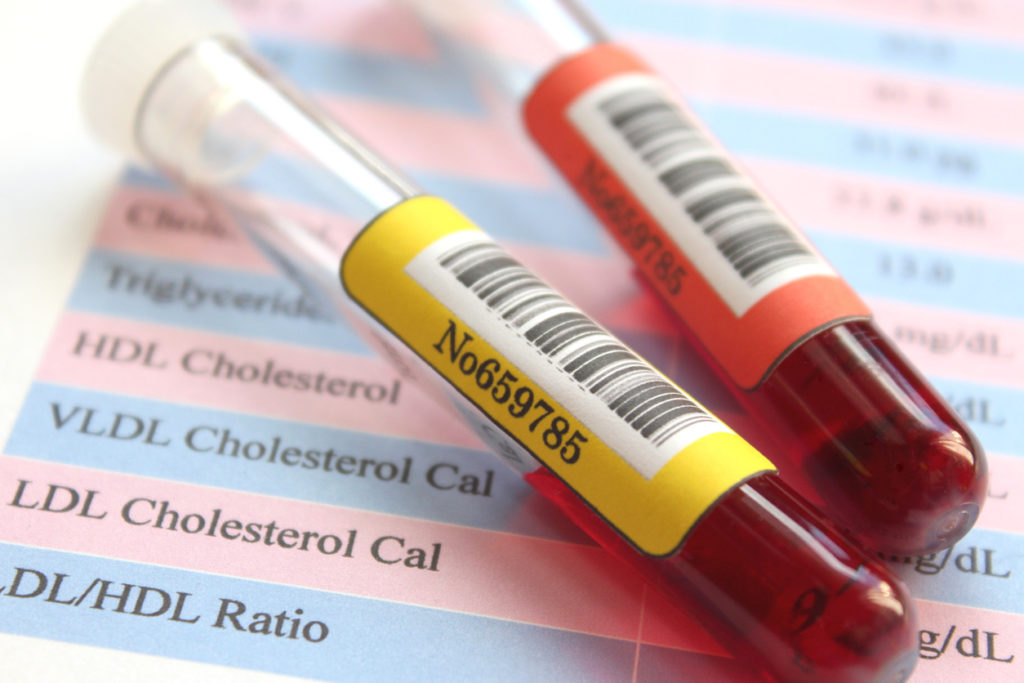
How can I find out my cholesterol levels?
The only accurate way to find out your cholesterol levels is to have blood drawn for a complete blood test. This test should examine your blood for triglycerides and HDL and LDL cholesterol. For accurate determination, you need to fast for 12 hours before having blood drawn – no food or liquids other than water. Quick cholesterol tests are becoming commonplace at health fairs and shopping malls. These quick tests may not always be comprehensive. It’s usually best to view these quick tests as screenings. That means you should follow them up with a complete blood test if the results indicate an unhealthy cholesterol profile.
If I have high cholesterol, will I have a stroke or heart attack?
Not necessarily. In general, the higher your LDL level and the more other risk factors you have, the greater your chances of developing heart disease or having a heart attack. Some people are at high risk for a heart attack because they already have heart disease. Other people are at high risk for developing heart disease because they have diabetes (which is a strong risk factor) or a combination of risk factors. Major risk factors that affect your LDL level include: diet, smoking, high blood pressure, low HDL cholesterol, family history of heart disease, age, obesity and physical inactivity.
If I have high cholesterol do I have to take medication?
Many people, after being diagnosed with high cholesterol levels, have chosen other treatments in lieu of medications. The class of medication most commonly used to lower cholesterol levels is statin drugs. The benefits of statins have periodically been overemphasized while the risks in many cases have been overlooked. It is not uncommon for individuals using statin medications to think that they now can have a diet and lifestyle that ignores their cholesterol levels – not true and might be dangerous! While statins have been shown to reduce cholesterol levels, they have also been shown to have side effects that include: muscle and joint aches, nausea, diarrhea, constipation, liver damage, and severe muscle problems that could result in possible kidney damage.
Will a low-fat diet help me reduce my cholesterol levels?
Beginning in 1993 and ending in March of 2005, the Women’s Health Initiative (WHI) enrolled 48,835 women, aged 50-79 years, in the WHI Dietary Study (also referred to as the Dietary Modification Trial). This study examined the effect of a low-fat (20% of calories), and high fruit, vegetable, and grain diet on breast cancer, colorectal cancer, and heart disease in postmenopausal women. The study diet focused on reducing total fat – and unlike diets recommended to reduce heart disease risk – did not differentiate between “good fats” (found in fish, nuts, and vegetable oils) and “bad” fats (like saturated fat and trans fat found in processed foods, meats, and some dairy products). The study design reflected a widely believed, but untested, theory that reduction of total fat would reduce risks of breast or colorectal cancers. For heart disease, it was anticipated that reduction in total fat would be accompanied by a reduction in saturated fats, which are thought to contribute to heart disease risk. Among the 48,835 women who participated in the trial, there were no significant differences in the rates of colorectal cancer, heart disease, or heart disease/stroke between the group who followed a low-fat dietary plan and the comparison group who followed their normal dietary patterns. Although the women in the study who reduced their total fat intake had a 9 percent lower risk of breast cancer than did women who made no dietary changes, the difference was not large enough to be statistically significant –meaning it could have been due to chance.
No Silver Bullet for High Cholesterol levels.
Those that are looking for a “quick fix” to their high cholesterol are out of luck. Your best option to maintain a healthy cholesterol level is through a nutritious diet (that includes plenty of dietary fiber) and some positive lifestyle changes (increased physical activity, decreased alcohol consumption, quit smoking, etc.).
In the United States, 32% of adult men and 27% of adult women have undesirable serum cholesterol concentrations contributing to cardiovascular disease, the number one cause of death. Achieving reductions in total and LDL cholesterol may be helped by adding to the diet psyllium, a dietary source of both soluble and insoluble fiber. Psyllium husks are the outer coating of the psyllium seed and are unique among dietary fibers for their positive effect on fecal bulking, among other things. In a meta-analysis of 8 different dietary studies, the University of Kentucky found that psyllium reduced serum cholesterol totals – as well as LDL cholesterol – over a treatment period of at least 8 weeks.
All 656 subjects in the 8 separate studies were hypercholesteremic and received psyllium in addition to their previously-prescribed low-fat American Heart Association “Step I” diet. All subjects consumed psyllium in the usual dose.
After 8 weeks of treatment, overall decreases in cholesterol levels were encouraging: LDL cholesterol was reduced 6.7%; and the LDL to HDL ratio decreased by 6.6%. The effect of psyllium appeared to focus on the reduction of LDL. In general, decreases in ratios of LDL to HDL cholesterol were greater in older subjects, with similar effects in both men and women.
The question of how psyllium works to reduce cholesterol is still under investigation, but the authors propose that psyllium fibers increase excretion of bile acid (derived from cholesterol) and secondarily increase the excretion of cholesterol from the liver.
Please note: If you are currently on a medication or a program for the treatment of high cholesterol, the information presented in this article is not to be used for anything other than educational purposes. Please feel free to present this information to your health care provider so you can both tailor your treatment program.
About the author:
Dr. Robert Irons graduated from the University of Missouri at Columbia with the first ever Ph.D. in Nutritional Immunology. He received postdoc training at the National Institutes of Health (NIH), National Cancer Institute (NCI) in the Nutritional Science Research Group. He has published in peer-reviewed journals such as the Journal of Nutrition, Journal of Infectious Disease, and Biochemical Journal and was an active health advocate on many health boards, such as NHF and PPNF. Dr. Irons was the former Vice-President of V.E. Irons, Inc. before sadly passing away in 2013.






No Comments